
Searching for the Doctor of shoulder replacement in West Delhi? No further look back, Dr. Raman Kant Aggarwalis the leading orthopaedic surgeon. Here gleno-humeral primary osteoarthritis is a progressive disorder characterized by damage to the articular cartilage of humeral head and/or glenoid. It can lead to debilitating functional limitations, compromising the individual’s quality of life leading to a signifcant socio-economic burden on the family and society, Shoulder replacement is the best option and the solution for such patients.
Reverse Shoulder replacement has become the preferred technique for treating neglected long-term cases of arthritis, tendon damage, fracture situations, or complications arising out of prior treatments or neglect. The procedure has become more popular as a result of more advanced implants, designs, and techniques, as well as a better understanding of the shoulder's biomechanics. Reverse shoulder replacement functions differently from conventional in that it does not require the stabilizing effect of the rotator cuff muscles, which are so important for conventional replacement to function.
Reverse Shoulder Arthroplasty has proven to be advantageous in the following conditions:
"The Medanta Institute of Musculoskeletal Disorders and Orthopedics" has a professional & dedicated shoulder and upper limb team which provides world-class care & treatment for arthroscopy and joint replacements of the upper limb. Our team of orthopaedic surgeons have performed more than 3,500 shoulder surgeries and over 200 shoulder replacement surgeries.
Here we present a case of complex primary shoulder osteoarthritis where a traditional anatomical replacement would have failed due to a deficiency in the shoulder socket (glenoid). A 65-year-old man came to Medanta complaining of right shoulder pain that had been getting worse over the course of two years. He had trouble moving his right shoulder and going about his daily business. He had been misdiagnosed as frozen shoulder and managed with analgesics and intra articular steroid injections elsewhere. The patient was experiencing pain even at rest; loading of the joint was also painful. He was a known hypertensive and had undergone knee replacement in the past.
The patient had internal rotation contracture of 30 degrees and a restricted range of motion, which prevented him from even reaching into his back pocket. Internal contracture prevented external rotation, abduction was at 70 degrees, and forward flexion was at 100 degrees. It was impossible to test the muscle strength because loading the arm was so painful. X-rays of the shoulder showed primary osteoarthritis, a Walch B2 biconcave glenoid, erosion of the posterior glenoid, and increased humeral retroversion. The humerus' head was posteriorly locked. So consult Dr. Raman Kant Aggarwal for your treatment of Reverse shoulder replacement in West Delhi.
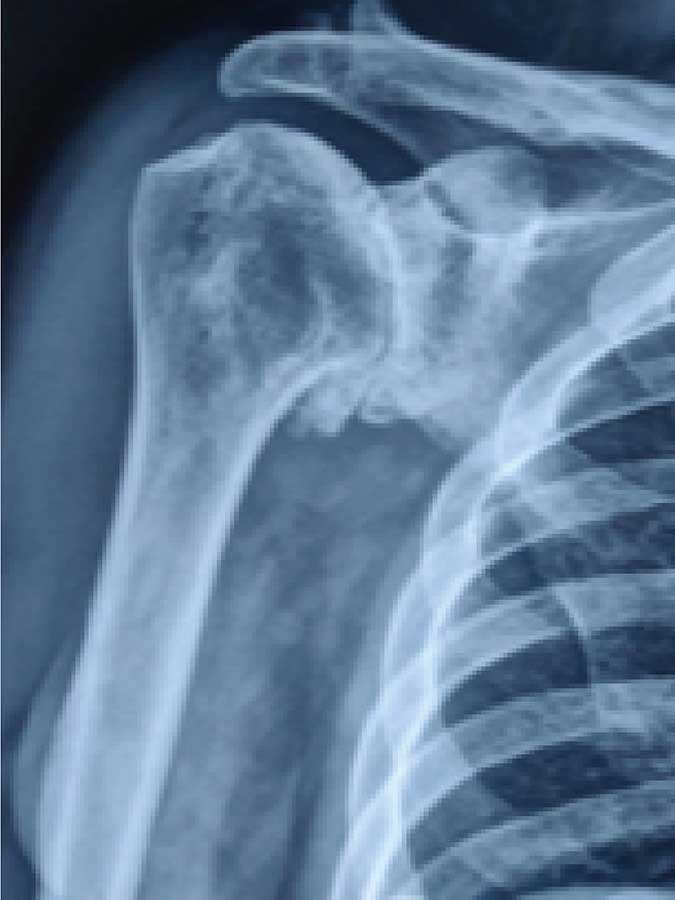
True AP view of shoulder showing Glenohumeral arthritis
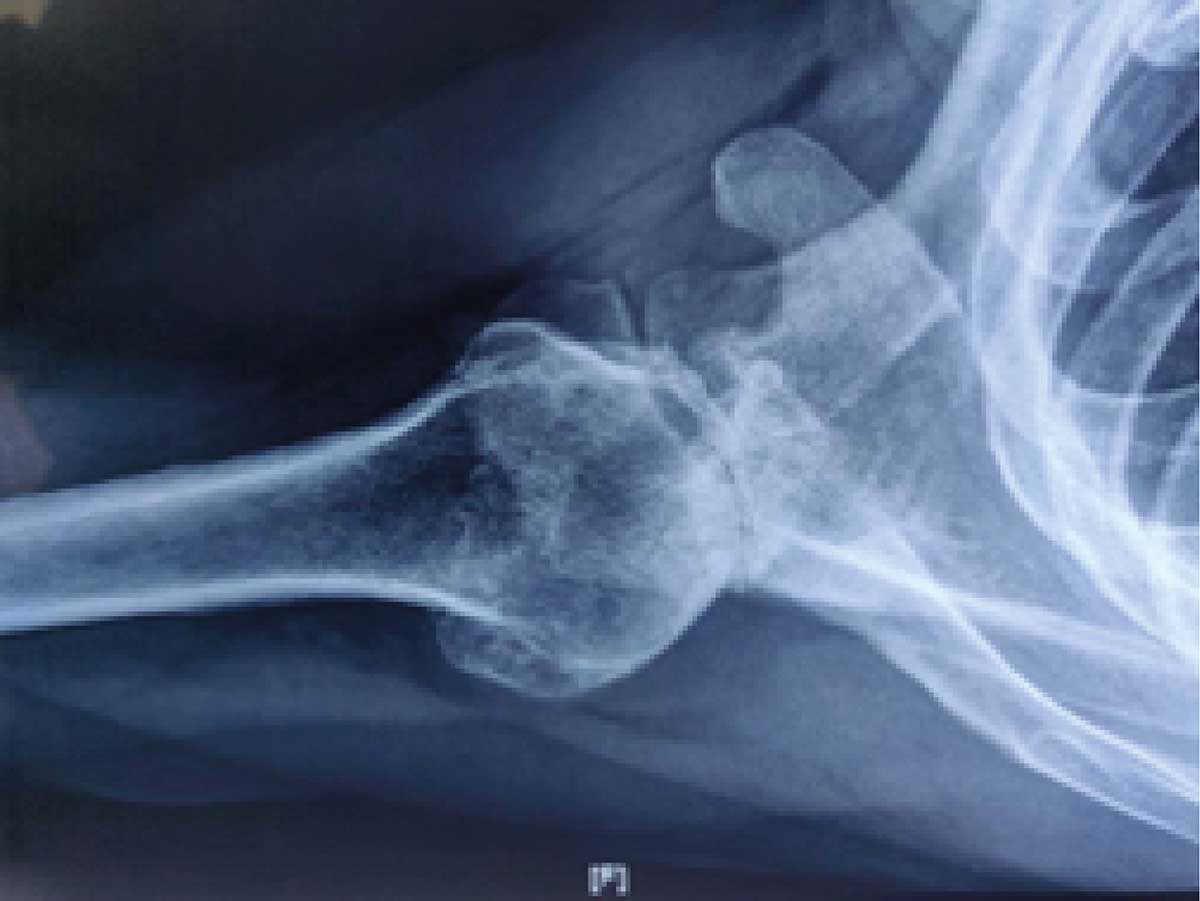
axillary view of the shoulder showing glenoid bone loss posteriorly, typically a Biconcave glenoid
CT scan was done to measure the exact bone loss on axial cuts, and get an estimate of wedge bone graft required to compensate for the glenoid defect to correct the native glenoid version.
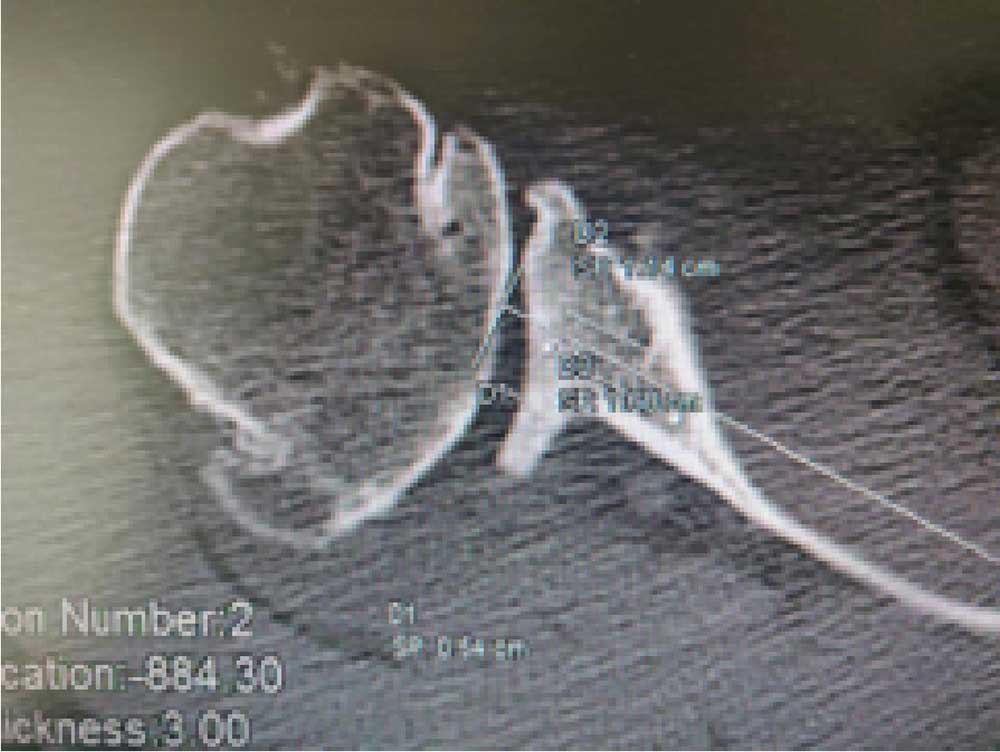
Axial CT cut showing arthritis and bone loss of glenoid
Pre-anaesthetic checkup of the patient was done and he was planned for Complex Reverse Shoulder Arthroplasty. The surgery was performed on the patient with biological restoration of the offset using a wedge bone graft from the humeral head.
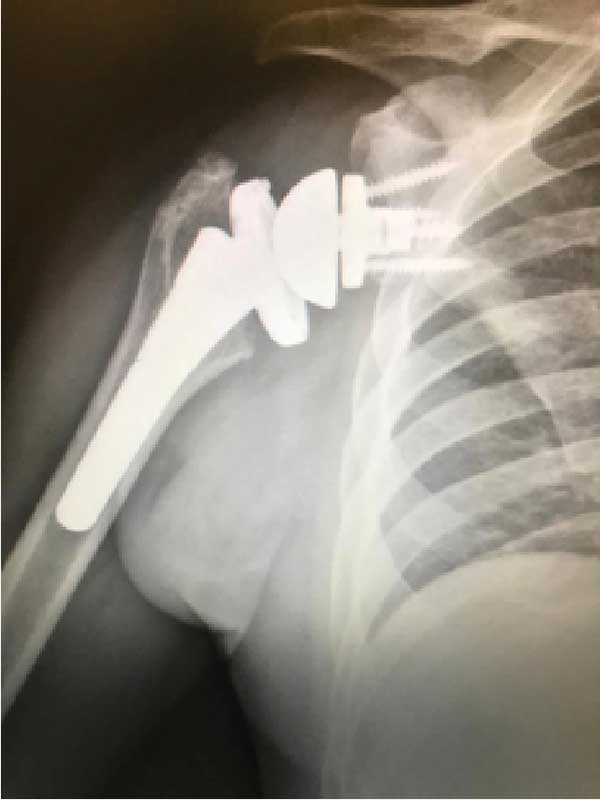
True AP view post operative
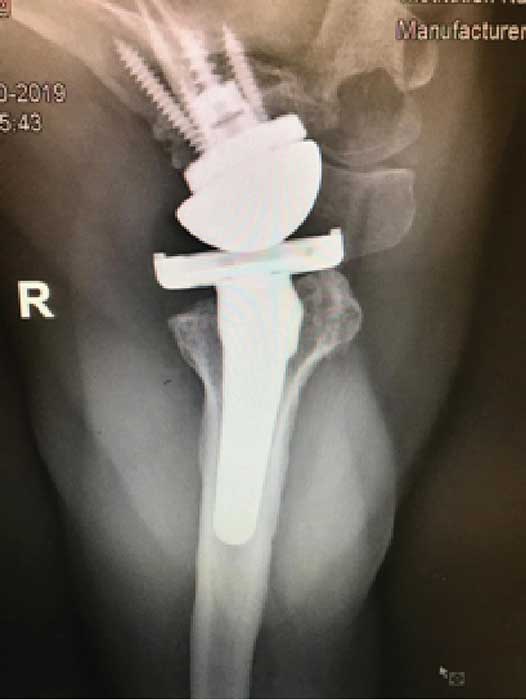
Axillary view post operative
The aim of Reverse Shoulder Arthroplasty is to restore painless functional joint which was achieved in this case despite the surgery being technically complex and challenging. 1.5 years post-op, the patient is doing well with stable, strong and pain-free shoulder.
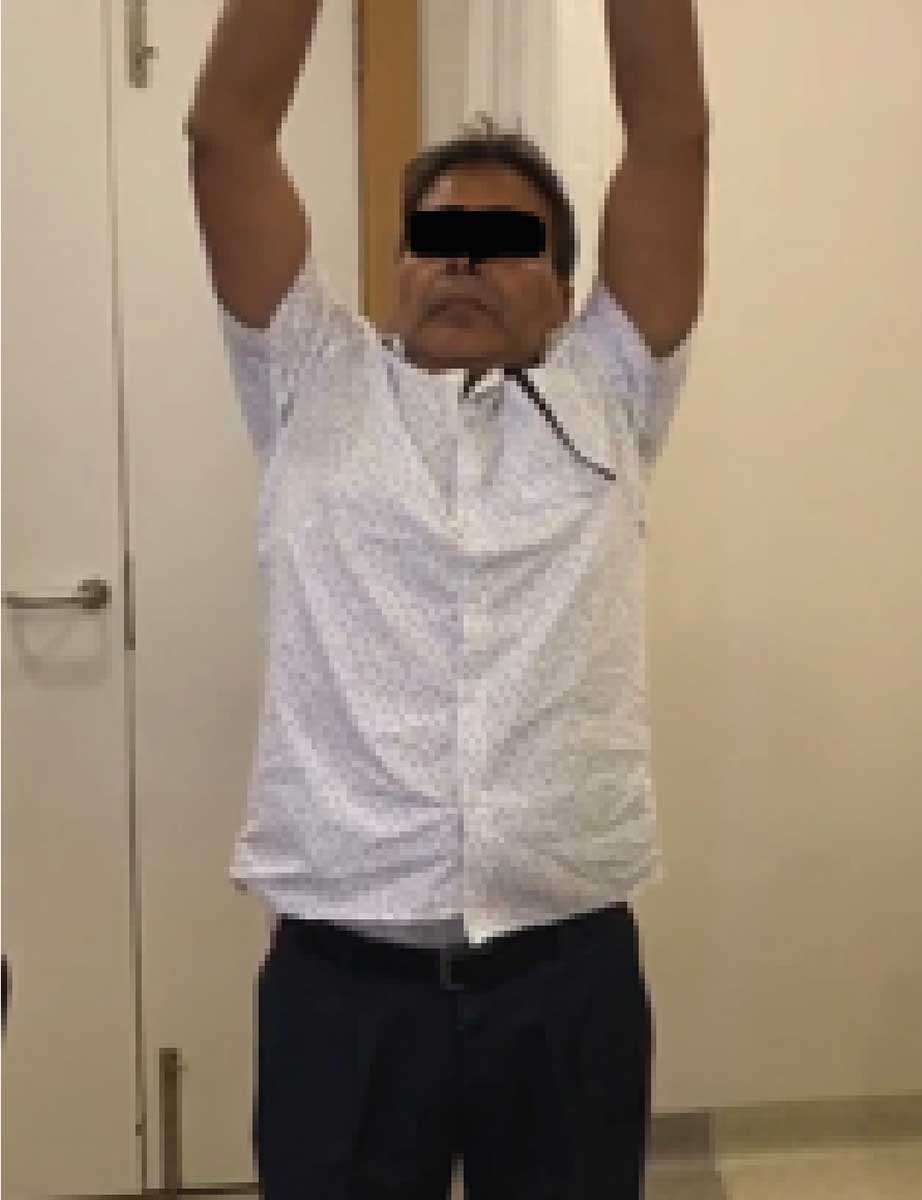
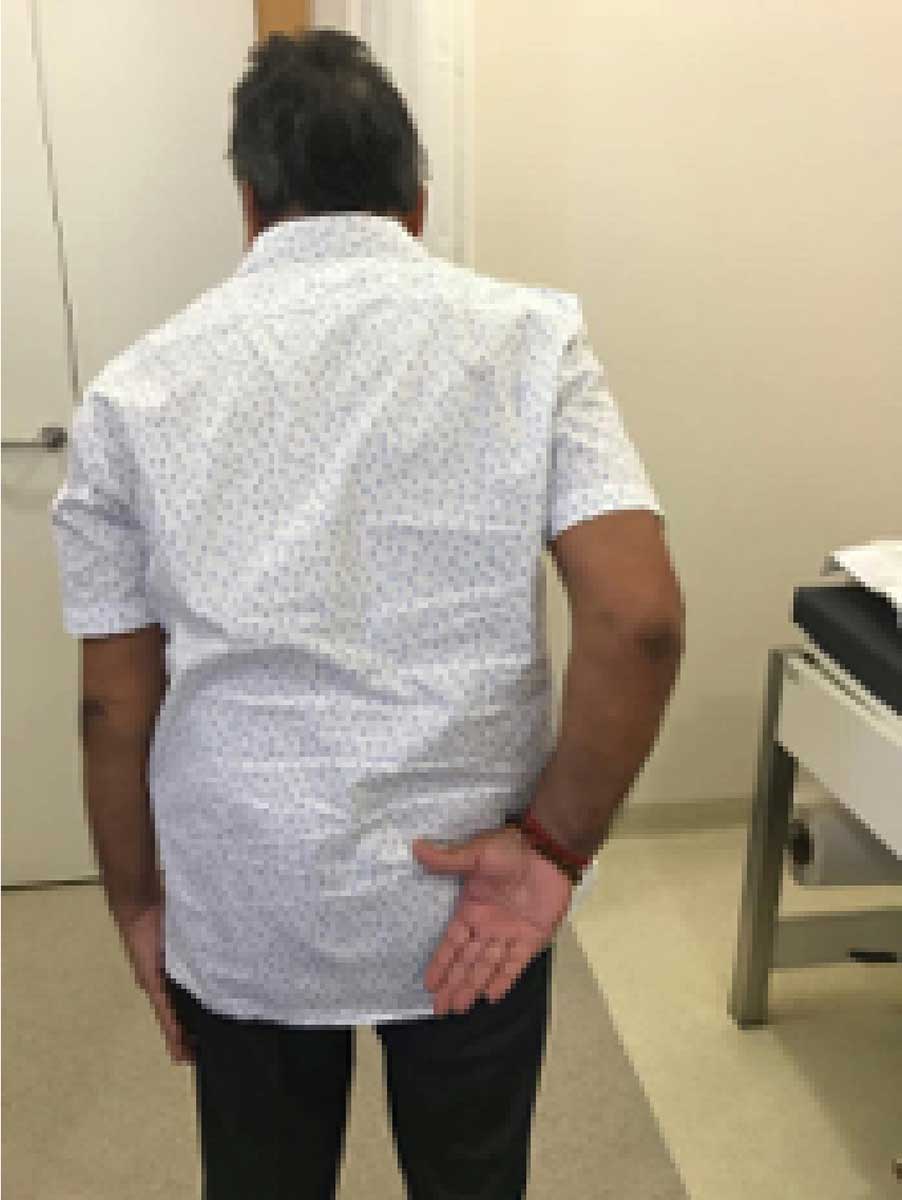
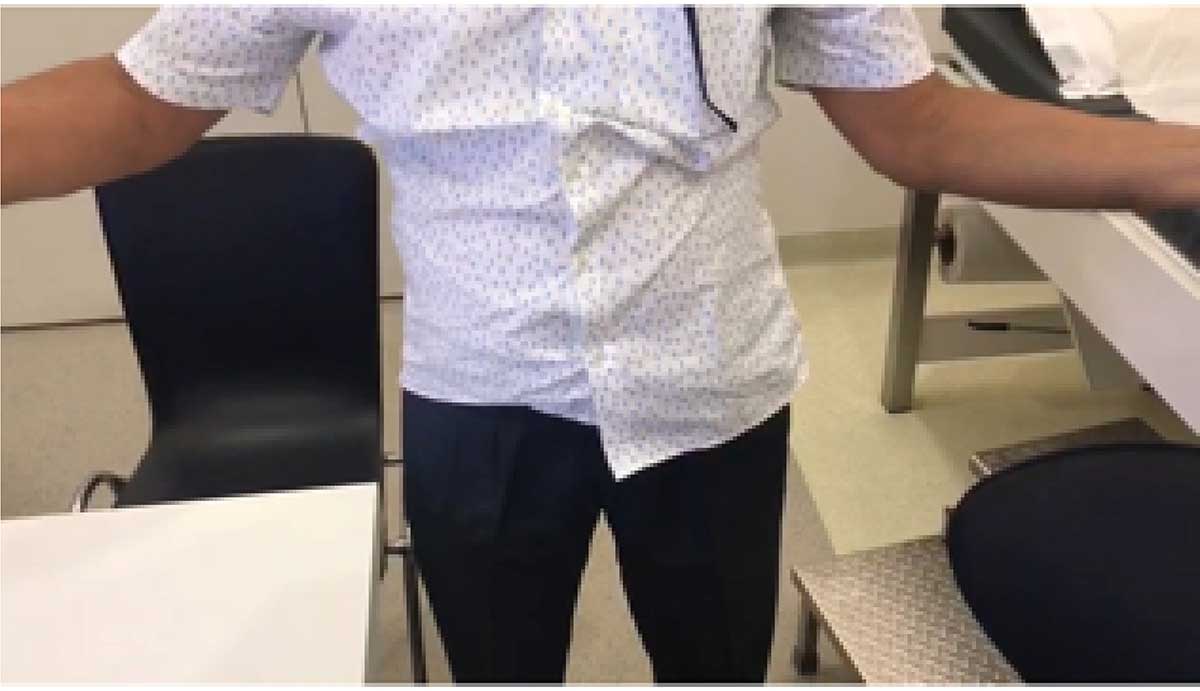
Post-op patient images showing functional range of motion indicating independence in performing activities of daily living.